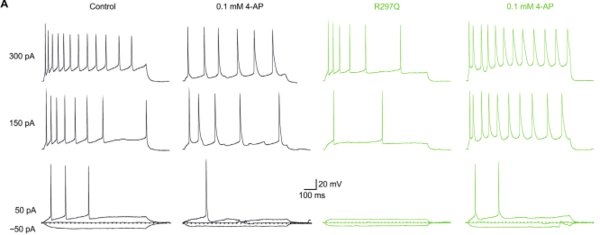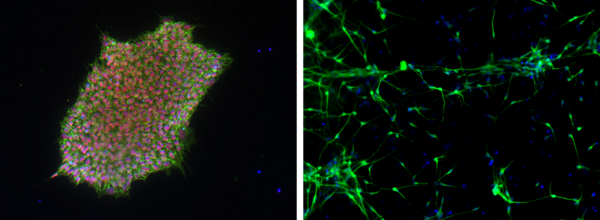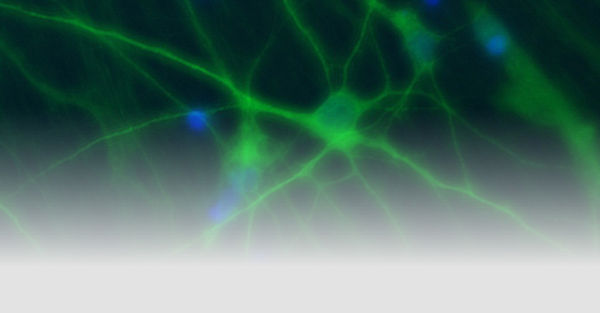
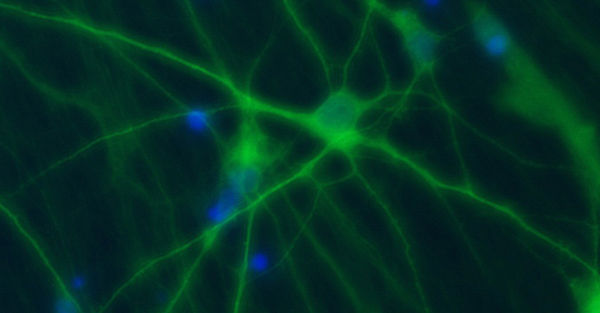
Ziel unserer Forschung ist es, die molekularen Mechanismen von hauptsächlich genetisch bedingten, neurologischen Erkrankungen, die durch eine abnormale neuronale Erregbarkeit verursacht werden, mit deren klinischen Symptomen und einer personalisierten Behandlung zu verknüpfen. Wir rekrutieren definierte Kohorten von Patienten mit Epilepsien und verwandten Erkrankungen, suchen mit modernen Sequenziermethoden nach krankheitsverursachenden Gendefekten, insbesondere in Ionenkanälen, Transportern und synaptischen Proteinen und analysieren deren funktionellen Konsequenzen, um die zugrunde liegenden Krankheitsmechanismen zu verstehen. Ein besonderer Schwerpunkt ist die Erforschung und Entwicklung neuer personalisierter Therapien für genetische Erkrankungen. Um die Mechanismen neuronaler Übererregbarkeit auf molekularer, zellulärer und Netzwerk-Ebene zu untersuchen, nutzen wir nicht-neuronale Modellsysteme wie automatisierte Messverfahren in Oozyten und Säugetierzellen, sowie neuronale Expressionssysteme. Letzteres beinhaltet die Generierung von Neuronen aus induzierten pluripotenten Stammzellen, die Verwendung menschlicher Hirnschnitte und genetischer Mausmodelle.

+49 (0)7071-
29-81921
Ausgewählte Publikationen
Müller P*, Takacs DS*, Hedrich UBS, Coorg R, Masters L, Glinton KE, Dai H, Cokley JA, Riviello JJ, Lerche H#, Cooper EC#. KCNA1 gain-of-function epileptic encephalopathy treated with 4-aminopyridine. Ann Clin Transl Neurol. 2023 Feb 15.
Krüger J, Schubert J, Kegele J, Labalme A, Mao M, Heighway J, Seebohm G, Yan P, Koko M, Aslan-Kara K, Caglayan H, Steinhoff BJ, Weber YG, Keo-Kosal P, Berkovic SF, Hildebrand MS, Petrou S, Krause R, May P, Lesca G, Maljevic S, Lerche H. Loss-of-function variants in the KCNQ5 gene are implicated in genetic generalized epilepsies. EBioMedicine. 2022 Oct;84:104244. doi: 10.1016/j.ebiom.2022.104244.
Boßelmann CM, Hedrich UBS, Müller P, Sonnenberg L, Parthasarathy S, Helbig I, Lerche H, Pfeifer N. Predicting the functional effects of voltage-gated potassium channel missense variants with multi-task learning. EBioMedicine. 2022 Jul;81:104115.
Johannesen KM*, Liu Y*, Koko M, Gjerulfsen CE, Sonnenberg L, Schubert J, Fenger CD, Eltokhi A, Rannap M, Koch NA,Lauxmann S, Krüger J, Kegele J, (…),Hedrich UBS, Benda J, Gardella E,Lerche H#, Møller RS#. Genotype-phenotype correlations in SCN8A-related disorders reveal prognostic and therapeutic implications. Brain 2021:awab321.
Auffenberg E*, Hedrich UB*, Barbieri R*, Miely D*, Groschup B, Wuttke TV, (…), Pusch M, Dichgans M, Lerche H, Gavazzo P#, Plesnila N#, Freilinger T#. Hyperexcitable interneurons trigger cortical spreading depression in an Scn1a migraine model. J Clin Invest 2021;131:e142202.
Hedrich UBS*, Lauxmann S*, (…), Bosselmann C, Schwarz N, Fudali M, Lerche H. 4-Aminopyridine is a promising treatment option for patients with gain-of-function KCNA2-encephalopathy. Sci Transl Med 2021;13:eaaz4957.
Koko M, Krause R, Sander T, Bobbili DR, Nothnagel M, May P,Lerche H; Epi25 Collaborative. Distinct gene-set burden patterns underlie common generalized and focal epilepsies. EBioMedicine 2021;72:103588.
Rosa F, Dhingra A, Uysal B, Mendis GDC, Loeffler H, Elsen G, Mueller S, Schwarz N, Castillo-Lizardo M, Cuddy C, Becker F, Heutink P, Reid CA, Petrou S, Lerche H#, Maljevic S#. In Vitro Differentiated Human Stem Cell-Derived Neurons Reproduce Synaptic Synchronicity Arising during Neurodevelopment. Stem Cell Reports 2020;15:22-37.
Schwarz N, Hedrich UBS, Schwarz H, P A H, Dammeier N, Auffenberg E, Bedogni F, Honegger JB, Lerche H, Wuttke TV, Koch H. Human Cerebrospinal fluid promotes long-term neuronal viability and network function in human neocortical organotypic brain slice cultures. Sci Rep. 2017 Sep 25;7(1):12249.

Hertie-Zentrum für Neurologie
Hertie-Institut für klinische Hirnforschung
Abteilung Neurologie mit Schwerpunkt Epileptologie
Hoppe-Seyler-Straße 3
72076 Tübingen
Tel.: +49 (0)7071 29-80466
Fax: +49 (0)7071 29-4488
Sabrina Kreiser
Yvonne Brändle
Tel: +49 (0)7071 29-80442
Fax: +49 (0)7071 29-4488
sekretariatne5.HL(at)med.uni-tuebingen.de
Heidrun Löffler
Tel: +49 (0)7071 29-81922
heidi.loeffler(at)medizin.uni-tuebingen.de